I will have to admit that when the National Wildfire Coordinating Group’s Risk Management Committee distributed some information earlier this year about rhabdomyolysis, which is frequently referred to as “rhabdo”, I didn’t pay much attention. But today when the Wildfire Lessons Learned Center announced that a Facilitated Learning Analysis (FLA) for a severe case of rhabdo was available, I read it carefully and am now converted. The injury in the FLA occurred September 21, 2011 while a firefighter was taking the Work Capacity Test, or “pack test”. I have seen the light and realize how serious this condition can be.
Left untreated, or if not treated early enough, rhabdo can lead to irreversible muscle damage, permanent disability, kidney failure possibly requiring lifelong dialysis, and even death. Up to 8% of cases of rhabdomyolysis are fatal according to a NIOSH report. And all of this can be the result of exercising hard or engaging in a strenuous fire assignment if other risk factors are also present.
Rhabdomyolysis is the breakdown of muscle fibers resulting in the release of muscle contents (myoglobin) into the bloodstream which are harmful to the kidneys and may lead to kidney failure.
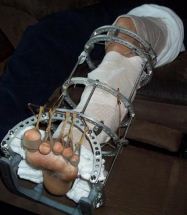
The link between rhabdo and “compartment syndrome”, the condition that is emphasized in the FLA, is certain, but it is not clear to me, having much more fire training than medical training, if compartment syndrome leads to rhabdo or vice versa, and my research found conflicting information. But that is not really important, in that both conditions are similar in that they are caused by damaged muscle tissue. Compartment syndrome occurs when the damaged muscle is inside an enclosed compartment in a fibrous sheath with other muscles, as is found in the arms and legs. Rhabdo can occur with any muscles, but both can lead to the same outcome, including death.
I was disappointed that the recently released FLA did not state the cause of the injured employee’s compartment syndrome/rhabdo, nor did it provide much useful information about how to prevent a similar occurrence, other than to “prioritize staying physically fit”, and the “incorporation of healthy lifestyle choices and better nutrition”. So I attempted to gather some information here in one place that will hopefully be useful for wildland firefighters, to increase their chances of avoiding rhambdo, or diagnosing it if it occurs.
Symptoms of rhabdo and/or compartment syndrome may include:

- pain out of proportion to what is expected
- muscle cramping
- tea-colored or cola-colored urine
- pallor (pale-colored skin)
- and later, paresthesia (a sensation of tingling, burning, pricking, or numbness of a person’s skin) and paralysis
The NWCG commissioned the National Institute for Occupational Safety and Health (NIOSH) to provide epidemiologic assistance, an “Epi-aid”, to determine the extent of rhabdomyolysis among wildland firefighters, and to identify possible risk factors unique to wildland firefighters. Here is an excerpt from the NIOSH report:
Since 2006, nine wildland firefighters with laboratory confirmed rhabdomyolysis and two with suspected rhabdomyolysis (not confirmed by laboratory testing) have been identified by direct communication between employers and the NWCG. Six have been reported since April 2010. Two firefighters are permanently disabled from complications from rhabdomyolysis. While there has been little research specific to wildland firefighters, we can recognize risk factors that may place them at increased risk for rhabdomyolysis. These include training and work activities such as high intensity load-bearing exercise, frequent eccentric muscle contractions (movements where muscle is attempting to lengthen and contract at the same time), altitude, dehydration, and high levels of ambient heat or humidity [Line and Rust 1995; George et al. 2010]. Because there is no surveillance system for identifying rhabdomyolysis cases in any of the five constituent agencies of the NWCG, it is likely that the cases identified for review as part of this Epi-aid represent only a proportion of cases of rhabdomyolysis among wildland firefighters.
The NIOSH scientists studied 10 cases in detail:
The 10 firefighters varied in age, type of wildland firefighter unit, assignment geography, symptoms, and outcomes. In half of the cases symptoms started on the first day of training, a new crew assignment, or the first day after completion of a fire response. The time between symptom onset and reporting of symptoms to supervisors varied from 30 minutes to 2 days. The time between symptom onset and arrival to a medical facility varied from 1 hour to 6 days. Five firefighters experienced disability for at least 3 months following discharge, and three of these have permanent disability.
And:
All identified cases of rhabdomyolysis occurred during or close to either training or actual fire response activities involving high levels of physical exertion, often carrying heavy packs. Despite carrying the prescribed water supplies, dehydration played a significant role in over half of the cases and several firefighters reported inability or considerable difficulty accessing their water supplies during physical exertion. Lack of acclimatization, use of medications or dietary supplements such as creatine, as well as caffeine intake, and other health conditions such as upper respiratory tract infections and flu-like illnesses also were likely contributing factors for the cases of rhabdomyolysis we reviewed.
The Niosh report lists these risk factors for rhabdomyolysis:
- overexertion
- poor conditioning
- heat stress/stroke
- dehydration
- prescription medications such as cholesterol-lowering statins and antidepressants
- over-the-counter medications such as antihistamines
- nonsteroidal anti-inflammatory medications and omeprazole
- excessive caffeine intake
- use of dietary supplements such as creatine and Hydroxycut (creatine is mentioned often in the literature as a major risk factor)
- use of toxins such as alcohol or amphetamine
- underlying medical conditions such as sickle cell trait or lupus
- concurrent acute viral illnesses such as influenza
Wikipedia lists these additional “common and important causes” of rhabdo:
- crush injury
- hyperthermia (high body temperature)
- hypothermia (very low body temperature)
- infection
- a hereditary muscle condition that increases the risk of rhabdomyolysis
Another excerpt from the report:
While it is not uncommon for individuals in the general population who engage in exertional activities higher than their baseline level of fitness to develop exertional rhabdomyolysis, it also occurs in highly-conditioned individuals who may engage in supramaximal exercise or who have other risk factors concurrent with an exertional activity.
More information:
- The FLA for the firefighter who was diagnosed following the Work Capacity Test (936 k)
- Information that a firefighter who has rhabdo symptoms should share with their healthcare provider, since many cases are mis-diagnosed. (a NIOSH product, large 7.8 Mb file)
- What wildland firefighters should know (a NIOSH product, large 2.5 Mb file)
- NIOSH report that was commissioned by the NWCG (76 k)
One more thing:
I commend the NWCG’s Risk Management Committee and their chair, Michelle Ryerson, for taking this issue to NIOSH who produced the report and the other publications listed above. And I hope the 2012 annual wildland firefighter refresher training spends at least 30 minutes on the topic.

Bill Arsenault,
Thanks for sharing the link to the new WildfireWorld from IAWF. It’s just the type of progress to spur me to renew my membership.
I first became aware of rhabdomyolosis while working behind the scenes for an organization helping a firefighter injured on the Basin Complex to get proper treatment, follow-up, and extended care through OWCP.
Having been on the ground level of a “forestry program” realizing an actual “EMS need” after the death of one of our firefighters in 1987, I started to speak out. I became an EMT in 1984 and could easily see the errors that contributed to our firefighters death.
During the mid-1990’s, after going through numerous hoops and challenges, our NF obtained BLS provider certification with the local EMSA.
Our NF now hosts (and staffs a cadre) teaching both EMT and Medical First Responder; has equipped our modules with state of the art BLS supplies; has an active AED program w/ AEDs on all modules (engines, crews, helitack); and participates regularly with the local EMSA of QA/QI programs.
Bill,
A number of articles and information have been published on this dangerous subject. IAWF requested an online article from me that was posted to http://www.wildfireworld.org on Rhabdo. “The New Dirty Word in Wildland Fire: Rhabod.”
Additionally, when wildland firefighters receive EMR or EMT training I include it in all my presentations. The only way to make more people educated is to have open discussions about it.
This will keep occuring if people do not take the time to become educated on the information.
If I can assist you in any manner in getting this information or you would like to see additional articles for understanding, please let me know.
Bill Arsenault
Wildland Firefighter/Paramedic
Release of myoglobin is also suspected as the cause of acute MIs (heart attacks) in healthy people, as well as the cause of injury/death from “crushing syndrome”.
Follow-up:
See –
http://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&sqi=2&ved=0CBoQFjAA&url=http%3A%2F%2Fwww.usuhs.mil%2Ffap%2Fresources%2Fet%2FExertionalRhabdomyolysis.ppt&ei=e-vETtCYBcSRiQKPqJDQBQ&usg=AFQjCNHuAifNSj9Apt-Qrnx190-iSfYq1g&sig2=yXLIL0Pmm6RX-SkRn9tU8g
http://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=2&sqi=2&ved=0CCIQFjAB&url=http%3A%2F%2Fwww.med.navy.mil%2Fsites%2Fnavmedmpte%2Fnmotc%2Fnami%2Fusnac2009%2FDocuments%2F1500%2520(THUR)%2520Gray%2520Navy%2520OAP%2520course%2520Rhabdo%2520presentation%2520Final.ppt&ei=e-vETtCYBcSRiQKPqJDQBQ&usg=AFQjCNGKKHv6LtmmIYr0EAPiilvWtT5wHQ&sig2=YzrFEudS3UJr-zY-jAh_Yg
http://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=2&sqi=2&ved=0CCIQFjAB&url=http%3A%2F%2Fwww.med.navy.mil%2Fsites%2Fnavmedmpte%2Fnmotc%2Fnami%2Fusnac2009%2FDocuments%2F1500%2520(THUR)%2520Gray%2520Navy%2520OAP%2520course%2520Rhabdo%2520presentation%2520Final.ppt&ei=e-vETtCYBcSRiQKPqJDQBQ&usg=AFQjCNGKKHv6LtmmIYr0EAPiilvWtT5wHQ&sig2=YzrFEudS3UJr-zY-jAh_Yg
Rhabdomyolosis is “compartment syndrome”.
No need to determine what came first, “the chicken or the egg”?. The terms are synonymous.
This is a serious problem that has been well documented (and recurring) within the wildland fire community… and it has very little to do with fitness, but rather more to do with unrealistic over-exertion; poor diets; & “dietary supplements” and “energy drinks” being consumed by firefighters on the fireline.
As stated before, there ARE serious problems with the WCT program… A program that has a similar number of serious injuries and deaths as burnovers and aircraft accidents.
Last count I have is 12+ deaths taking or preparing for the WCT since its introduction to “IMPROVE SAFETY”. Probably ten-fold the number of serious injuries.